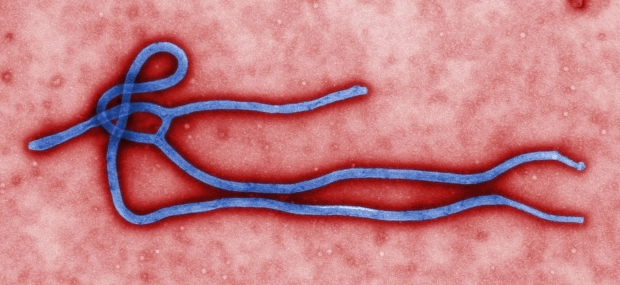
Ebola virus virion, created by microbiologist Cynthia Goldsmith.
“This current Ebola outbreak is intellectually interesting but at the same time a little bit frightening because we’re at the front line, but this is what we went into this area of medicine for." – Dr David Holland, Middlemore Hospital’s Clinical Director Infection Services
Lisa Thompson finds out how Middlemore, one of New Zealand's largest hospitals, is preparing for Ebola.

Left: Dot McKeen, Middlemore Central Manager and Dr David Holland, Middlemore Hospital’s Clinical Director Infection Services, inside the hospital’s new bio-containment unit
Right: Inside the Middlemore Hospital’s new bio-containment unit opened at the beginning of October 2014
While the Ministry of Health assessment is that the risk to New Zealand from Ebola remains low, one of the country’s largest hospitals is not taking any chances. Middlemore Hospital in South Auckland has just opened a bio-containment unit, which is reserved for any patients who are suspected carriers of the virus.
According to the Auckland Regional Public Health Service's ill-traveller protocol, Middlemore is obliged to take ill patients arriving at Auckland International Airport as it is the closest hospital. Given its proximity to the airport, Middlemore Central general manager Dot McKeen said Counties Manukau Health is taking the lead on planning. “We as a group had been together talking about flu and how we manage it, so when we were alerted to Ebola, we already had that good knowledge and working relationships in place.”
A vacant neonatal care unit caught the eye of Dr David Holland, Middlemore Hospital’s Clinical Director Infection Services, and within a week it was converted to the bio-containment unit. It’s currently set up to receive two patients but Dr Holland says it can be easily enlarged. “We’re only using a fraction of the space we have available. I call it an aircraft carrier deck of space to work with, but if we need to expand we could convert further space for another three patients.”
While currently devoid of any human activity for now, the expansive wing has been fully stocked and fitted with medical equipment, computers and personal protection gear including gowns, visors, protective suits and boots. The unit is divided into three zones – green, orange and red and will be monitored by the infection control team and nursing staff.
The green zone is for changing into protective gear, as well as being a clinical and observation room, with a large window allowing clinicians to observe the patient without having to go into their room. The orange zone acts as a “decontamination” area and the red zone is the unit’s main patient quarters.
Security guards would be posted at the entrance to the unit and would screen anyone trying to access it. Dr Holland says a team of managers and infectious disease clinicians are meeting weekly to iron out protocols in the hospital if a patient is suspected of Ebola. “There’s four infectious disease physicians and a microbiologist as well as four or five infection control practitioners and if the call goes out, we’ve decided everybody arrives – even at three in the morning.”
He says staff are also undertaking regular training around how to get into and out of personal protection equipment. And once a clinician has carefully undressed after seeing the patient, the items will be bagged and then double bagged before disposal to a “Rotoclave”, a machine that breaks down and sterilises waste before it is incinerated. The unit is currently set up to receive two patients in two separate negative pressure rooms.
While each room contains a bed, a computer for patient records, a toilet, sink and television, Dr Holland says the red zone is being kept as bare as possible as any new item that is introduced to the room, has to be removed, sterilised and destroyed. Family members and other clinicians will be able to communicate with the patient via an intercom.
And while the unit may never receive a suspected Ebola case, Dr Holland says it’s a great asset for Middlemore to have. “We can deal with other infectious agents such as a SARS outbreak should it occur, and that’s the silver lining if you like, we have a facility that we can use in the future.”
More about Ebola preparation at Middlemore Hospital, including a video tour.
Ebola facts
Information gathered from the New Zealand Ministry of Health, the World Health Organization and the Centers for Disease Control and Prevention.
- Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, is a severe, often fatal illness in humans.
- The illness affects humans and nonhuman primates (monkeys, gorillas, and chimpanzees).
- Ebola first appeared in 1976 in two simultaneous outbreaks, one in a village near the Ebola River in the Democratic Republic of Congo, and the other in a remote area of Sudan.
- The current outbreak in West Africa, (first cases notified in March 2014), is the largest and most complex Ebola outbreak since the Ebola virus was first discovered.
- As of October 15 close to 4,500 people have died from the disease in West Africa, mainly in Liberia, Sierra Leone and Guinea.
- The United States has also had two confirmed cases and in October, a nurse in Spain became the first person to contract the virus outside of West Africa.
- The United Nations has also confirmed that a medical officer attached to the UN Mission in Liberia, has died from Ebola while being treated in a hospital in Germany.
- The World Health Organisation is warning that the outbreak could grow to 10,000 new cases a week within two months.
- Ebola virus is not spread through the air and is not spread through casual contact.
- It requires contact with infected body fluids (such as blood, saliva, urine or faeces) through broken skin or mucous membranes (such as the mouth or eyes).
- You can also become infected by coming into direct contact with objects contaminated with the virus or with infected animals.
- Ebola can only be spread to others after symptoms begin, which can appear from 2 to 21 days after exposure.
- Symptoms include fever, headache, diarrhoea, vomiting and muscle pain.
- The Ministry of Health assessment is that the risk to New Zealand from Ebola remains extremely low.
For more information please head to Ministry of Health: Ebola update

