While Youthline and Lifeline struggle to stay afloat, leaving calls for help unanswered, the government is funding a brand new helpline.

Photo: Illustration: Lee Smith-Gibbons / The Wireless
A teenage girl sends a text to 234. She's suicidal.
The message pops up on a computer screen in Youthline's Grey Lynn, Auckland "hub" and Angela*, a voluntary triage counsellor, responds immediately.
Texts between the two go back and forth.
It's a cold, rainy Wednesday* evening, about 9pm, and the girl is staying with her uncle in Napier.* She tells Angela via text message that she was raped by a friend, and she is not coping. She has a plan to kill herself.
Angela swivels her office chair to her left and chats with her colleague Elena*, who is sitting in the tiny booth next to her. They are the only two people in the country who are manning Youthline's phones this evening. Usually it's just Elena.
They decide they need to intervene to save the girl's life. Angela messages her, asking how she feels about involving police. Does she want them to come? Will she give Angela her address?
The girl agrees, Angela calls 111 and two police officers are dispatched to her home. Hopefully they arrive in time.
***
Last year, Youthline received more than 18,000 phone calls and 126,000 incoming text messages from young people across New Zealand. One in three contacts related to suicide, depression, self harm and anxiety. But Youthline is so underfunded - the only government funding it received this year was $90,000 from Oranga Tamariki - that between 30 and 40 percent of calls go unanswered.
It's not the only helpline struggling to keep helping. Last year, Lifeline, which also runs Kidsline and suicide crisis helpline Tautoko, received about 126,000 calls, but answered only 54,471 of them. That means more than 71,500 cries for help went unanswered.
Yet while Youthline and Lifeline struggle, in June last year the then Health Minister, National's Jonathan Coleman, launched 1737 - Need to Talk? - a brand new, fully government funded service, providing a 24/7 text and telephone helpline. In the 12 months since its launch, 1737 has received 18,237 calls and conducted 19,736 conversations by text message (the number of text messages is measured very differently by 1737 and Youthline, and is therefore not easily comparable). Most of their contacts come from young people, aged 13 to 24.
Though 1737 sounds strikingly similar to both Youthline and Lifeline, the big difference is that it is funded via a multi-million dollar contract with the Ministry of Health. Andrew Slater, chief executive of the National Telehealth Service, which runs 1737, says all New Zealand's mental health helplines are different, and all appeal to different demographics.
But Youthline spokeswoman Briana Hill says it's frustrating to see a government funded service being established from scratch, when Youthline, which was founded in Auckland in 1970, is so well recognised by young people as the go-to helpline, that it's overwhelmed with calls it's unable to answer.
***
It costs about $800,000 a year to keep Youthline's phone, text, email and webchat lines running. Most of that money comes from corporate sponsors and donations, and Youthline's helpline has never had any major government contracts. It relies mostly on volunteers to answer the phones.
Meanwhile, cries for help from people in New Zealand are becoming increasingly urgent. In the last 10 years, the number of mental health related 111 calls to police increased by 88 percent. The number of suicide related calls to police increased by 141 percent over the same period.
And the stakes are high - New Zealand's youth (15 to 24-year-olds) suicide rate between 2009 and 2012 was the highest among 34 OECD countries. The suicide rate for Māori youth in 2012 was 48 per 100,000 compared with the non-Māori youth rate of 16.9 per 100,000. In the five years from 2012 to 2016, 20 Māori youths aged 10 to 14 killed themselves - that's 60 percent of all deaths in that age group.
In 2015, Ministry of Health mortality data shows that suicides accounted for 33 percent of deaths (111 of 339 deaths) among 15 to 24-year-olds (deaths by suicide accounted for about 2 percent of deaths across all age groups.)
In the 12 months from July 2016 to June last year, the suicide rate for 15 to 19-year-olds was 12 in 100,000 and 22 in 100,000 for 20 to 24-year-olds, according to provisional statistics released by the coroner.
A government inquiry into mental health and addiction describes the mental health system as being underfunded and is currently looking into ways of tackling New Zealand's "stubbornly high suicide rates." A spokesman for the inquiry says its terms of reference are broad, so if questions about mental health helplines are raised, the panel will consider them.

Photo: Illustration: Lee Smith-Gibbons / The Wireless
***
In her 2012 PhD thesis, Ailsa Haxell writes of a boy hiding under his house: He is waiting for his drunk father to go to sleep. He picks up his cellphone. He can't call - his dad will hear him talking - so he sends a text message to 234. Soon, he gets a response from a Youthline counsellor. They ask if he'd like to call for free.
"Um i dnt lik to tlk on phnes cause ma dad will give me a hiding," he replies.
He and the counsellor chat for a while via text instead, until his dad goes to sleep and it's safe to go inside again.
Another Youthline user tells a counsellor she's being pressured into having sex with her boyfriend: "bt i dnt no if im redi".
"I wana tel u afwl thngs," writes another.
"Hae um I dnt reail knw wat to say but um i been realy depressed / n cutn wrist n dnt knw wat to do. HELP!!!"
A man is making his way along a bushy track. He's looking for a cliff to throw himself off. He takes out his phone and sends a text to Youthline.
"They can try and make me feel good," he later tells researchers Kerry Gibson and Claire Cartwright, who are studying the helpline.
He has lived to retell this story. But what if no one had been there to reply?
When Elena is working Youthline's phone lines alone each night, she is often swamped - sometimes juggling calls, texts and emails at the same time. At 6pm on the rainy Wednesday, she is texting two people who have overdosed, and two others at risk of suicide.
The Grey Lynn hub is a cluttered and homely workspace. Pink streamers are draped across the backs of computer screens, blue and white balloons lie in clumps on plush grey couches and brightly coloured paintings and notices are tacked on to the walls.
But around 10pm, when the lines are the busiest, Elena is usually on her own in the grey-carpeted, cream-walled booth. If she's on a call when another person tries to phone in, she can't pick up.
***
At the Wellington branch of the Samaritans helpline, volunteers answer between 20,000 and 25,000 calls a year. But another 20,000 to 25,000 calls go straight to voicemail.
They too rely on volunteers, and receive no money from government contracts.
Bernadine Reid of the Samaritans' Wellington branch says securing funding, recruiting and retaining volunteers is a continual struggle.
"The phone line is often busy. There are daily callers who want to talk to us for hours. The goal is for no call to go unanswered. At the moment, more than half the calls are not picked up."
She says the helpline's struggle is just a symptom of much bigger problems faced by vulnerable New Zealanders.
"What we are doing is linked to the mental health services. Helplines do help. But maybe what would be more appropriate for many of these people is what is not available. Some callers need to be in hospital. But they're not - they're out in the community and they have to resort to calling us."
Lifeline cost $6.3 million to run last year (the organisation also offers other helplines, training and specialist counselling services). In 2015, it lost two of its major government contracts - the Sir John Kirwan-fronted Depression Helpline and the Gambling Helpline. Lifeline tendered for the contract to continue running those helplines, but pulled out at the last minute. This resulted in the organisation facing a reduction in income of about $3.5m a year, and the closure of its text and webchat services.
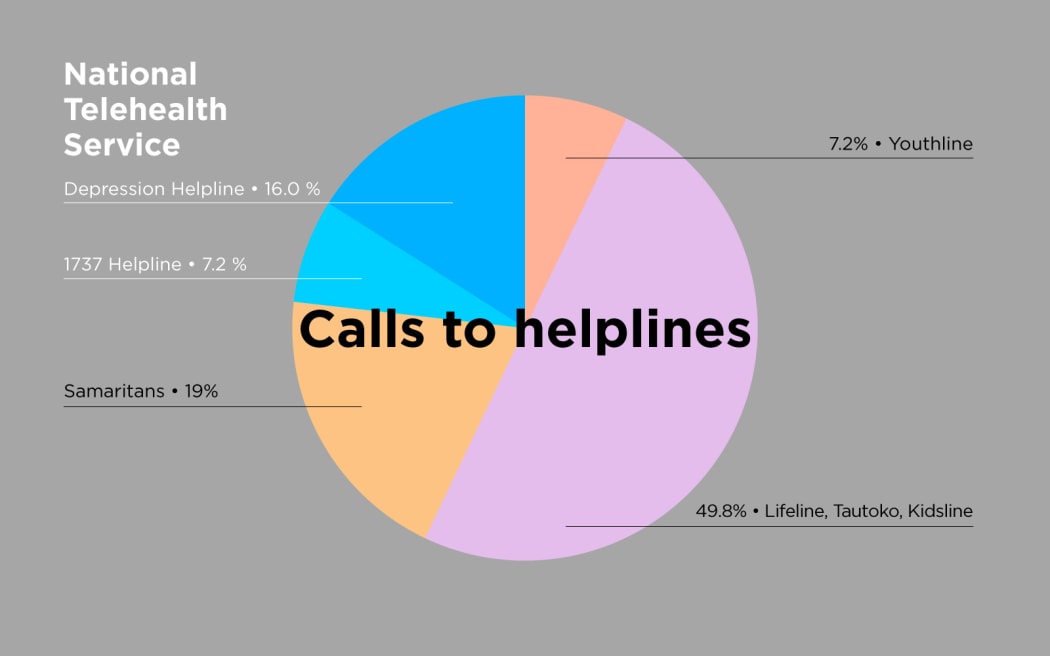
Photo: Graphic: Luke McPake / The Wireless
James*, who worked at Lifeline for four years, says that within about three months of the service losing its contracts, between 12 and 14 staff left. "It was sudden. It changed the spirit of the organisation," he says.
But the loss of funding didn't result in a reduction of people calling in, Lifeline executive director Glenda Schnell says, and in March this year, with corporate funding, they relaunched a free text support service - HELP (4357).
***
The money Lifeline had previously used to run the gambling and depression helplines went to new kid on the block National Telehealth Service, run by social enterprise Homecare Medical.
So why fund a new helpline while the old guard struggles for cash?
In the lead up to New Zealand's 2011 General Election, the National Party made a campaign promise to consolidate 11 telephone healthline services, which received close to 2 million contacts a year.
The idea was to reduce pressure on after hours primary care services, ambulance services and hospital emergency departments. Callers could be "seamlessly" transferred from one service to another, and the government hoped that by consolidating the services, it would create a greater public awareness of what was available.
There was also a significant financial benefit to come from the consolidation. A 2013 cabinet paper released under the Official Information Act shows the Ministry of Health spent about $49m each year on these 11 telehealth services - that's $490m over 10 years. Under the new plan, the government would spend $258m over 10 years, saving about $232m.
The contract to set up and run the National Telehealth Service was awarded to Homecare Medical in 2015. The service now operates a total of 14 helplines. As well as 1737, the Depression Helpline and the Gambling Helpline, it runs Healthline, Quitline, the Alcohol Drug Helpline, the National Poisons Centre, the Immunisation Advisory Centre and an ambulance secondary triage clinical hub, which takes non-emergency 111 calls. It also runs online services The Journal and The Lowdown and this month launched the sexual harm helpline Safe to Talk He pai ki te kōrero.
Across the 14 helplines over 10 years, that's an average of $1.8m per helpline each year. (We don't know how the money is actually distributed among the lines - the National Telehealth Service says it's hard to say, and the Ministry of Health says it does not know.)
After the launch of 1737, Health Minister Jonathan Coleman said the line would make it easier for people to connect with mental health and addiction specialists working within the National Telehealth Service.
"It's one number, easy to remember, that's a gateway to a range of phone-based services. At the moment, there's a range of numbers people have to call," he said in June 2017.
In the 2016/17 year, the National Telehealth Service answered more than 79 percent of calls within 20 seconds, and the helplines provide a good service; more than 90 percent of callers surveyed said they were satisfied or very satisfied with the help they received.
The organisation's head, Andrew Slater, says 1737 filled a gap in the helplines market, and takes a similar approach and tone to community conversations around mental health.
"It's more about 'give us a call if you need to talk'. We've got a team of mental health professionals who are all professionally trained counsellors, psychologists, psychotherapists, social workers, who are here 24 hours a day to talk to you. And if you don't want to talk, give us a text - because we understand that's how young people want to engage. So that service is very aimed at starting that conversation."
A spokesperson for the Ministry of Health said "information the Ministry has received" indicated that 1737 was reaching people who might not otherwise seek help.
A woman who has texted in to 1737 for help, told The Wireless her experience was a positive one. "You definitely feel like you're talking to a person and not a robot. The messages were friendly and mostly timely, I think I didn't have to wait very long for the person to reply, so it felt like texting a friend. The responses were empathetic without being pretentious, they asked some probing questions to get a better understanding of [my] situation, and they gave a couple of practical tips - she recommended a women's multivitamin and seeing a face-to-face counsellor."
But the multi-million dollar pool of government money that 1737 has access to, and the similarity of its service to Youthline's, has left Youthline spokesperson Briana Hill frustrated. She doesn't mind that other helplines present a choice of services for clients. It's the equality of funding - or lack thereof - that she finds difficult to reconcile.
"[It] can be really challenging for us, having worked in this space for 48 years now, seeing newer initiatives spring up that are very similar or the same as what we already offer," Hill says.
"I could understand if we weren't meeting a need, or if people weren't connecting with us."
But the numbers show this isn't the case, and Colmar Brunton research from 2014 found Youthline was the most "salient" youth support organisation among 16 to 24 -year-olds in New Zealand.
"If people need to reach us they know who we are," Hill says.

Photo: Illustration: Lee Smith-Gibbons / The Wireless
***
One of the National Telehealth Service's noble, but lofty future goals is to "provide a safety net for those affected by mental health issues and societal disadvantage."
But despite the government's hope that the service would take the pressure off emergency services, by consolidating helplines and creating greater public awareness of the ones available, figures from police and ambulance show that people in crisis situations are increasingly calling 111 instead.
Last year, police received more than 27,000 mental health related calls to 111, and almost 22,000 calls relating to suicide threats or attempts.
Acting inspector Matthew Morris, police national manager of mental health and community services, says there is no simple answer as to why these numbers are going up so steadily. "What we face in New Zealand in regards to calls to emergency services going up... is certainly nothing unique," he says.
"There's no one definitive answer for why people are calling us. It's probably things like increased social isolation, increased feelings of financial pressure, substance abuse, family harm, there are a range of different things... it is many combining factors."
The near universal recognition of the 111 number is likely one such factor, he says. "We are a well known number and people, when they call us, they know that we provide a 24-hour, seven-day-a-week service and often we will turn up in person. That's one of the key factors you have to remember - for some people, they want to talk to someone face-to-face, and that's why they call us."
Police are now training staff on how to recognise people who are in distress or at risk of suicide. They also provide legislation training, and experts and mental health users are brought into the police college to speak to recruits.
***
So what can be done to help the helplines give clients the support they need, when they need it?
For Youthline to be able to answer more calls, the simple solution, according to Hill, would be more money.
"It's frustrating to know that we could be doing more, and we just can't based on what we have."
Youthline's goal is to answer at least 80 percent of all calls, and they're working hard to make it happen. But Hill says they need money to employ more people, so that two counsellors like Angela and Elena are working from 8pm to midnight every night.
In the meantime, users who can't get through to the traditional helplines are likely to get a response if they contact 1737. The numbers show that the use of the helpline is increasing, despite the service only spending about $18,000 on marketing and advertising in the last 12 months. Slater says this is a deliberate measure to ensure counsellors are able to answer all the calls they receive. Each time the service gets a mention on the TV news, or they run a Facebook ad campaign, they see a jump in users (they often put on extra staff in anticipation) and Slater is wary of triggering a level of growth that is unsustainable: "It would be irresponsible of us to market and advertise the service and not have the capacity to answer those calls," he says. Slater says it's important that the service maintains its clinical integrity - that callers and texters are always connected with professionals who can help.
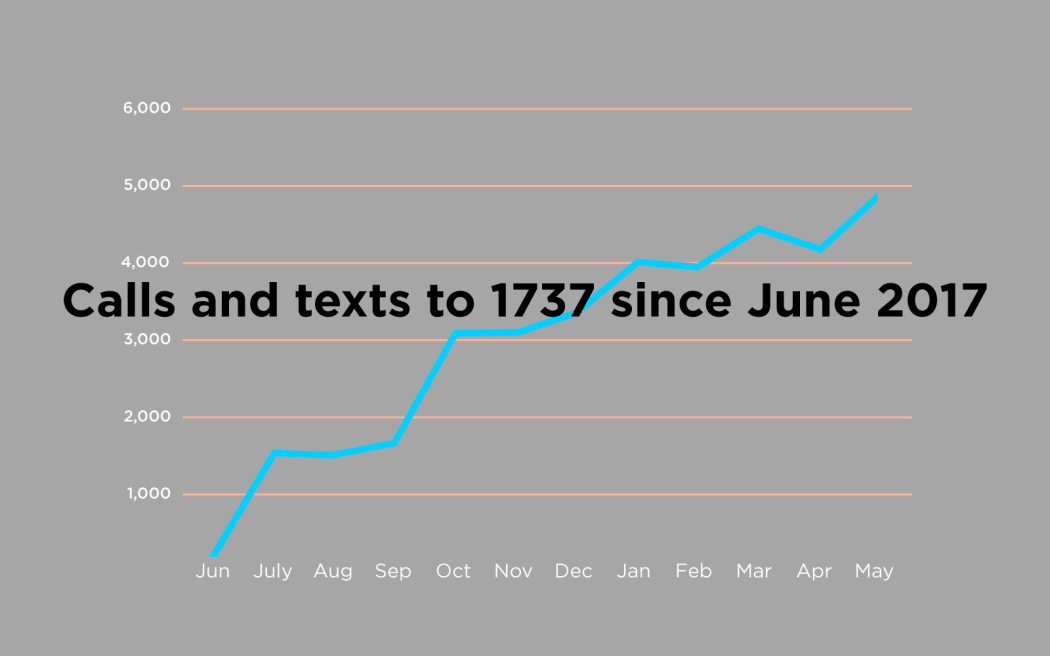
Photo: Graphic: Luke McPake / The Wireless
In a written statement, a spokesperson for the Ministry of Health said the Ministry recognises the services Lifeline, Youthline and Samaritans provide to people experiencing mental distress.
"People will seek support in many ways which can include volunteer helpline organisations," the spokesperson said. "One of the strengths of the National Telehealth Service is that people who contact the service through any phone line or any communication channel are able to talk to professional staff and receive the most appropriate service to meet their advice and support needs."
When asked if there were plans to help fund the services, the Ministry did not directly respond.
Health Minister David Clark would not be interviewed, and did not respond to written questions for this story. His press secretary indicated that he was being careful with his public comments while the inquiry into mental health and addiction was underway. Clark is a supporter of the 1737 helpline, though, and can often be seen wearing its logo on the lapel of his jacket.
The Mental Health Foundation's chief executive Shaun Robinson also refused to comment. "We don't wish to be drawn into a comparison of these services," a spokesperson said via email.
***
Although Elena is one of the few paid staff working Youthline's phones, some days she chooses to volunteer time too. When asked why, she sounds earnest when she answers that she does it for love. But it can be hard, she says.
"A lot of the people that contact us are struggling. There can be a lot of pain that is shared, but it is an incredibly beautiful journey to be able to be alongside that person when they really, really need it. Even if you can't help, you know you've listened and they've had somebody who has absorbed what they've said and cared."
Elena says the tenuousness of Youthline's income is scary, as is the thought that people, like the girl who texted in on that rainy Wednesday night, might not get an immediate response.
She says that teen's cry for help on that night was not out of the ordinary. Youthline gets similar calls and messages almost every day. If Elena is on her own and a call comes through while she's on another line, that caller misses out.
It's not nice for her to think about what happens when there's no one there to talk.
*Names and identifying details have been changed to protect the privacy of Youthline clients and staff members. The Wireless was granted access to Youthline's Grey Lynn hub and its counsellors on the condition that the privacy of clients remained paramount.
***
Where to get help:
1737 - Need to Talk? Free call or text 1737 any time to speak to a trained counsellor, for any reason.
Lifeline: 0800 543 354
Suicide Crisis Helpline: 0508 828 865 / 0508 TAUTOKO (24/7). This is a service for people who may be thinking about suicide, or those who are concerned about family or friends.
Depression Helpline: 0800 111 757 (24/7)
Samaritans: 0800 726 666 (24/7)
Youthline: 0800 376 633 (24/7) or free text 234 (8am-12am), or email talk@youthline.co.nz
What's Up: online chat (7pm-10pm) or 0800 WHATSUP / 0800 9428 787 children's helpline (1pm-10pm weekdays, 3pm-10pm weekends)
Kidsline (ages 5-18): 0800 543 754 (24/7)


