The decision to have a child can be life changing. But Kate* says she didn’t have a choice.

Photo: Lucy Han / The Wireless
A woman who was denied a second trimester abortion through North Shore Hospital says the ordeal was so traumatising, she contemplated suicide.
Kate, a 28-year-old administrator, was 18-weeks and five days pregnant when she was referred by her GP to the Waitematā District Health Board for a second trimester abortion.
But the day after her referral, she says she was called by a social worker who told her doctors were not comfortable with performing a termination after 18 weeks.
New Zealand law states that an abortion can be performed up to 20 weeks under specific circumstances when approved by two licensed doctors who are called “certifying consultants”.
If a woman is more than 20 weeks pregnant, an abortion can be legally performed to save her life or prevent serious permanent injury to her physical or mental health.
But second trimester abortions require a high level of medical expertise and are only available in some areas. In the Auckland region, they are usually done by specialists from private practices, under contract to district health boards (DHBs).
Kate says she was told by the Waitematā DHB social worker that Auckland District Health Board’s (ADHB) Epsom Day Unit would also refuse to do the procedure.
However, a report from ADHB notes that 35 second trimester terminations were performed last year, 17 of which were performed at 18 or 19 weeks. Between 2010 and 2016, two terminations were performed at 20 weeks and one at 21 weeks.
A spokesperson for the Abortion Supervisory Committee, which is legislated to oversee the administration of abortions in New Zealand, said if a DHB does not do terminations up to a certain gestation, they have a duty of care to refer the woman to a hospital that can provide the procedure.
But instead of being referred to ADHB, Kate was told she would have to seek a termination in Australia, a procedure that would cost her more than $9000.
According to Waitematā DHB policy, surgical terminations won’t be agreed to from 18 to 20 weeks gestation, despite what the law says. The policy states women wanting a termination at this gestation must be advised that they can have a surgical termination in Australia at their own cost.
“If however there are serious mental health risks or physical abnormalities identified for the in-utero baby then a referral should be made to [certifying consultants’ names redacted] for discussion. They can consider offering a medical termination at North Shore Hospital,” the policy reads.
Kate says she was never offered this option.
***
Kate and her partner were on holiday in Bali when she discovered she was pregnant.
The couple had been drinking alcohol, and Kate was concerned about the effect this would have on the foetus. She was told by a local doctor that she was likely in the first trimester of her pregnancy (up to 12 weeks).
“I didn’t realise I was pregnant, and I had been drinking quite heavily,” Kate said. She had just recovered from a depressive episode, and said she probably have missed an oral contraceptive pill during this time.
“I had no symptoms [of pregnancy], I wasn’t exercising and I ate badly - so I just put weight gain down to that .”
Due to Kate’s mental health issues, and her concerns for the health of the foetus, she and her partner considered accessing an early medical abortion pill while in Bali. But instead, she said they decided to “do it by the book” and seek a termination upon their return to New Zealand.
“We trusted the New Zealand healthcare system, never expecting it to let us down like this.”
***
On Monday, August 21, after visiting her Auckland GP and learning that she was in fact into the second trimester, Kate was referred to the Waitematā DHB. The following day, she received a call from a social worker.
Kate says she was told by the social worker that a team of certifying consultants were not comfortable with performing a surgical termination at 18 weeks. The social worker told Kate she would need to go to Australia for the procedure.
At 3.48pm, Kate received a text message from the social worker:
“Hi Kate, so sorry to have to inform you that you are unable to assist you with your request [sic]. Please look at Marie Stopes Org in Australia who will be an option for you.”
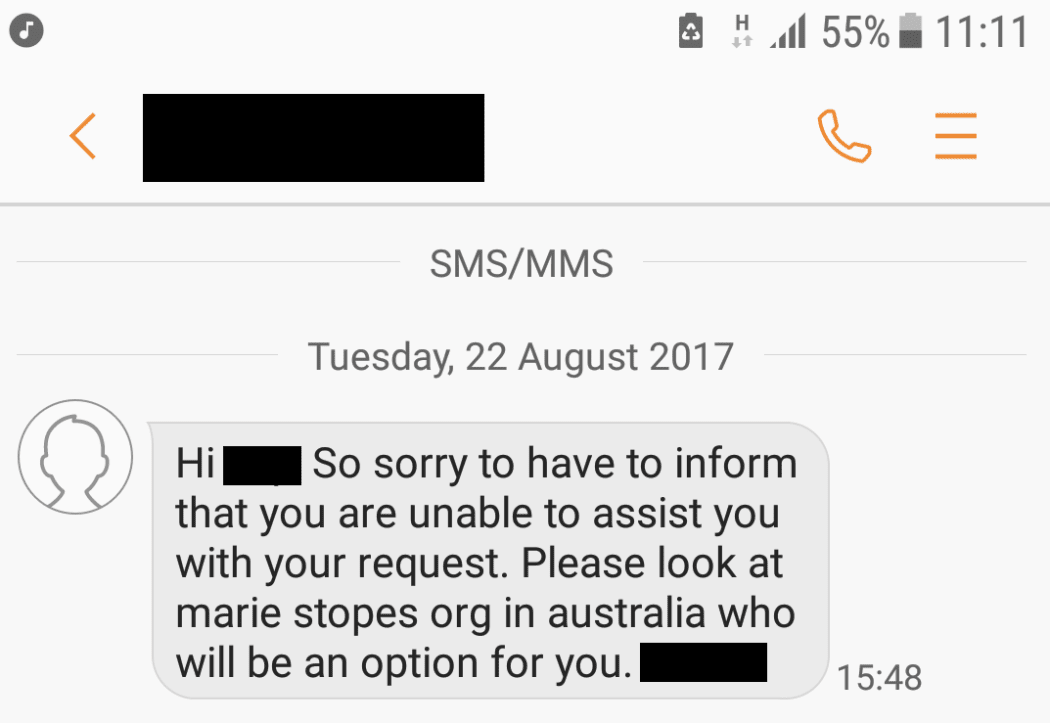
Kate was told by text message to seek a termination in Australia. Photo: Unknown
As a New Zealander, a late term abortion through Australia’s Marie Stopes costs $4390 at 18 weeks, $5000 at 19 weeks and $9100 at 20 to 23 weeks and six days. Kate said she was told by the social worker that the Waitematā DHB would not contribute to the cost of an overseas termination.
Kate responded to the text message asking to speak with the doctors. This request was ignored, until the following day when she was given the names of three doctors at a private clinic in Remuera to which Waitematā DHB outsources some terminations.
But Kate said she was told by the social worker that the doctors would not be confronted by distressed people, and therefore would not speak with her.
Kate immediately called her GP and asked to be referred to a different DHB.
In the meantime, she contacted Marie Stopes, extended her mortgage by $10,000 and took leave from work so she could travel to Australia.
On Wednesday, August 23, Kate was granted an appointment with a social worker at the Epsom Day Unit for August 28 - one week after she first saw her GP. When she visited the clinic she was 19 weeks and five days pregnant.
At Epsom Day Unit she was told by a social worker that ADHB did provide second trimester terminations. But by this stage, Kate said the stress of her ordeal had almost overwhelmed her, and she had come to a decision not to have an abortion.
“I always knew that New Zealand's abortion laws were not the most progressive, but this experience really opened my eyes to just how distressing going through the whole process was,” she said.
“A decision to terminate was never made lightly, and I am sure you can understand the enormous impact children have on one's lifestyle, finances, and physical and mental health.
“Yet I had that decision taken away from me.”
Because she believed ADHB would also turn down her request for an abortion, she and her partner said they had begun working towards accepting she was having a baby. But not by choice.
“We were made to change our minds, we were made to come to terms with it.”
Kate said that during time she spent trying to arrange a termination, her mental health suffered to the point where she considered self harm or suicide as a way of escaping what she called a “desperate situation.”
She has made a formal complaint to the Waitematā DHB.
In a meeting with Kate last week, DHB staff denied she was told Epsom Day Unit would not do the procedure. Kate was also told that it was Waitematā DHB policy not to do surgical terminations from 18 weeks gestation.
A doctor in the meeting told Kate that he would refuse to perform a termination at or past 18 weeks unless that person had “major psychiatric issues” and was on antipsychotic medication, even if a psychiatrist had determined a pregnancy would be detrimental to her mental health.
A spokesman for the DHB told The Wireless there was a thorough process for handling complaints, but he would not comment on specifics until an investigation was completed and a detailed response was given to Kate.
However, in the meeting with Kate, she was told by Waitematā DHB that the social worker contacted Kate’s GP who allegedly said he thought her mental health was not at risk due to her pregnancy - meaning she could not legally have an abortion under New Zealand legislation.
By law, however, the decision of whether or not an abortion can be performed based on mental health grounds is to be made by two certifying consultants, and not a GP.
The president of the Abortion Law Reform Association of New Zealand (ALRANZ), Terry Bellamak, says according to Kate’s story, she was prevented from seeing a certifying consultant.
“The Crimes Act allows abortions up to 40 weeks, but applies stricter criteria for abortions after 20 weeks than before 20 weeks. On what legal basis does the Waitematā DHB restrict abortions to 18 weeks? On what legal basis does the DHB refuse to allow a woman the opportunity to have her case considered by certifying consultants?”
She said Kate’s experience was a horrific demonstration of how New Zealand’s abortion laws were not working.
“Kate’s life has been changed forever. It is outrageous the law’s inconsistent application is allowed to mess people’s lives up like this.”
***
Kate is now 22 weeks pregnant.
She says she wasn’t ready to have a baby. She wanted to be able to plan, to save and to ensure her mental health was sound enough to bring up a child.
She felt fortunate to be in a good financial position, and was able to extend her mortgage. But she worried for women who weren’t in the same position as she was financially - which is why she chose to share her “traumatic” experience.
She and her partner are struggling to find a midwife, and still have serious concerns about the effects of alcohol on the foetus.
*Kate and her partner have chosen to remain anonymous to protect their future child’s privacy.
***
Where to get help:
Need to Talk? Free call or text 1737 any time to speak to a trained counsellor, for any reason.
Lifeline: 0800 543 354
Suicide Crisis Helpline: 0508 828 865 / 0508 TAUTOKO (24/7). This is a service for people who may be thinking about suicide, or those who are concerned about family or friends.
Depression Helpline: 0800 111 757 (24/7)
Samaritans: 0800 726 666 (24/7)
Youthline: 0800 376 633 (24/7) or free text 234 (8am-12am), or email talk@youthline.co.nz
What's Up: online chat (7pm-10pm) or 0800 WHATSUP / 0800 9428 787 children's helpline (1pm-10pm weekdays, 3pm-10pm weekends)
Kidsline (ages 5-18): 0800 543 754 (24/7)
Rural Support Trust Helpline: 0800 787 254
Healthline: 0800 611 116
Rainbow Youth: (09) 376 4155
If it is an emergency and you feel like you or someone else is at risk, call 111.


