A veteran midwife has questioned the relative benefits of stem-cell harvesting from umbilical cord blood, saying growing evidence shows a natural, physiological birth gives a baby the best chances of future health.

Photo: 123RF
Dr Maggie Banks, who is based in Hamilton, said a newly-released report showed further evidence that delayed cord clamping benefited the neurological development of infants and pointed to possible negative effects of immediate cord clamping after child birth.
The New Zealand College of Midwives also urged hospitals that didn't put adequate emphasis on delayed clamping to do so immediately in light of the report's findings, published in The Journal of Pediatrics this month.
Delayed clamping allows the natural transfusion of blood from the placenta to the baby until the cord stops pulsating.
The report, led by pioneering American midwife Dr Judith Mercer, found clamping delayed for five minutes significantly increased brain myelin in four-month-old infants.
Myelin is an insulating substance made up of protein and fatty substances that forms around nerves, including those in the brain and spinal cord.
The myelin sheath allows electrical impulses to transmit quickly and efficiently along the nerve cells.
Ferritin, a protein that contains iron levels, was also found more abundantly in the infants who had their cord clamping delayed, instead of clamping immediately.
The study found a positive relationship between ferritin and myelin.
Immediate clamping, a practice routinely used in the past, still happens in hospitals, including when blood is collected from the placenta for stem-cell harvesting so this material can be used to help treat illnesses the child may develop in the future, like cancer.
Previous data had already shown delayed clamping resulted in a 30 percent increase in blood volume and a 50 percent increase in iron-rich red cell volume, whereas immediate cord clamping likely contributed to iron deficiency in infancy.
The current report noted that studies in animals clearly linked a lack of myelin with iron deficiency and neurodevelopmental impairment, and that "abnormal myelination is associated with a variety of childhood developmental disorders, including dyslexia and autism spectrum".
The randomised trial of 73 pregnant women and their babies was conducted at the Women and Infants Hospital of Rhode Island and Brown University in the US between 2012 and 2016.
The study showed infants randomised to the delayed cord clamping group had greater myelin content in the internal capsule and other early-maturing brain regions associated with motor, visual, and sensory function.
The study said "ethical concerns regarding comparisons to immediate cord clamping" should be considered.
"Given that delayed cord clamping is a feasible, low-tech, no-cost approach, it has the potential to have widespread impact on early life development," it said.
Stem cell harvesting
Dr Banks, who had spent 40 years working in women's health, agreed and said women seeking to pay for blood collection from the placenta, so their baby's stem cells can be harvested and stored, should be fully informed on the issue.
Private medical company CordBank, which has a medical facility in Auckland, collects and stores cord blood for parents so material can be used to treat possible illnesses that could rise during their child's lifetime.
Parents who have signed up to the scheme see it an "insurance policy", with one parent on the company's website saying they wanted to give their children "the best start in life".
The website said the process didn't take important blood away from the baby.
"Cord blood is normally discarded with the umbilical cord after it is cut," it states.
"When you ask to have your baby's cord blood collected, the one and only change from the normal procedure is that after birth, after the cord is cut, the baby's cord blood is collected rather than thrown away."
Dr Banks questioned the claim.
"It is wrong to say that, this is a manipulated process where the baby is being denied blood it would have otherwise received during a physiological birth," she said.
"Any intervention in the natural physiological process effects the baby and must be very considered.
"With some newborns it may take 30 seconds for the cord to stop pulsating and the placenta blood transfused into the baby. For others it may take 45 minutes. The baby is given what it needs."
She said the benefits of allowing the blood to drain from the cord into the baby were evidence-based and the latest report added to that growing understanding.
In contrast, CordBank's commercial scheme of stem cell collection and storage offered the possibility of a treatment for limited illnesses that may arise in a person's lifetime, she said.
She said there was more of a focus here on collecting data to benefit emerging methods of treatment, many of which were still being trialled. But ultimately, it was the choice of parents on what they thought best for their child.
CordBank founder and chief executive Jenni Raynish told RNZ cord delayed cord clamping and stem cell collection were not mutually exclusive and that enough blood could still be harvested if the delay was between 30 to 60 seconds.
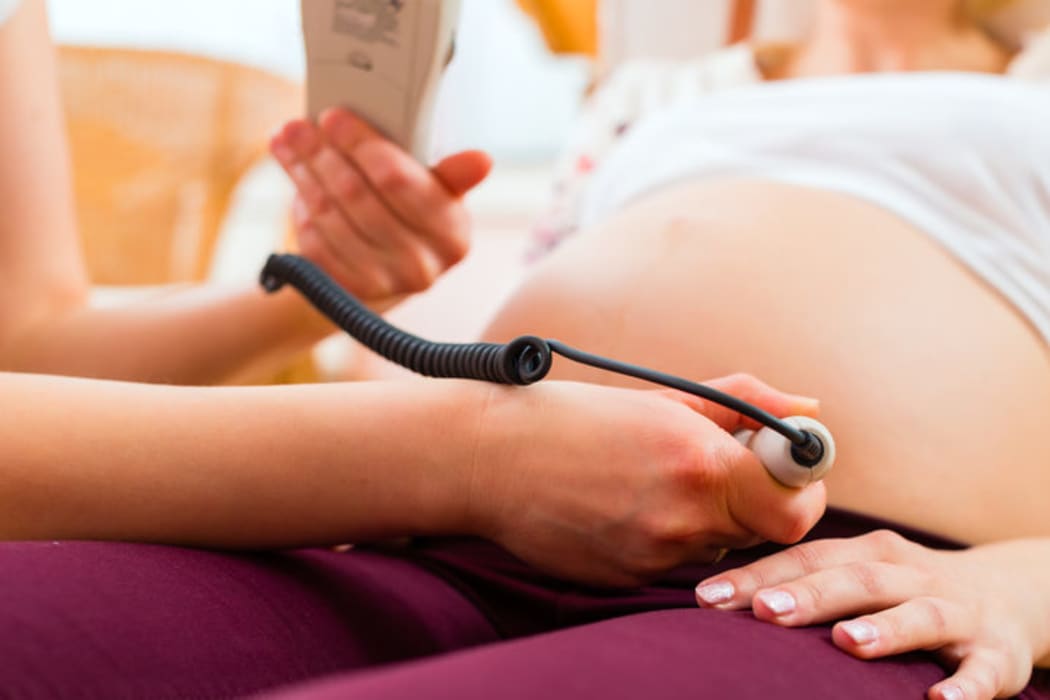
Photo: 123RF
She said evidence of successful stem-cell treatment for illnesses like cancer was overwhelming and parents saw the value in opting for the pharmaceutical investment.
"After a baby is born, the umbilical cord is clamped and cut," she said.
"This may be done immediately after birth or it can be delayed, and different groups have different opinions on how long to wait...
"The independent international website Parents Guide to Cord Blood Banking states that studies show that most of the blood transfer from the umbilical cord to the baby occurs in the first 60 seconds and that medical professionals consider delayed cord clamping to be waiting 30 seconds or more after the birth."
The company said it had 7000 'primary maternity carers' on its books to collect placenta blood.
It is understood primary maternity providers receive a fee of $150 from CordBank to drain the umbilical cord blood.
The company charges a fee of $2900 to collect and cryogenically store the blood. An annual storage fee of $225 applies. The material is discarded or "given back" if the fee is not paid.
Hospitals must respond - midwives
The New Zealand College of Midwives told RNZ any interference with the third stage of child birth needed to be a considered decision to "support best outcomes for both mother and baby".
"Evidence of probability of any benefit for routine private cord blood collection needs to be explained to prospective parents in an unbiased manner," college researcher Lesley Dixon said.
She said the new study added to evidence demonstrating the benefits of delayed cord clamping.
"Any hospitals that don't currently put emphasis on delayed clamping should do so in light of these findings," she said.
She said midwives supported undisturbed third stage labour, where the cord was left intact until it stopped pulsating, generally between 10 and 20 minutes.
She said this happened with approximately 35 percent of women and babies in New Zealand each year.
"The importance of not interfering with a woman's natural physiology during birth is becoming increasingly understood and validated through research studies such as this but it has taken many years for this midwifery perspective to be respected," she said.
"In the meantime the longer-term effects and potential harms of routine interventions during childbirth are yet to be fully uncovered."
RNZ contacted all district health boards across the country, with most saying hospitals used or attempted to use delayed clamping in their maternity departments as circumstances allowed.


